Lichen planus (or lichen ruber planus) is usually a chronic inflammatory dermatosis, the aetiology of which is caused by an autoimmune-type reaction, usually manifesting as flat pustules, 2/4mm in size, scaling and reddish skin eruptions, generally circular in shape, often accompanied by itching. It affects about 1% of the population globally and predominantly affects women between 50 and 70 years of age.
There are basically two sites on which lichen can occur: the dermis or the mucous membranes.
In terms of the skin, lichen can occur on:
- skin folds (wrists, ankles, forearms or lumbar region).
- lower limbs, in the leg region. In such a case, we speak of ‘hypertrophic’ lichen because these papules tend to fuse together (thus generating what we can call ‘plaque’ since its maximum diameter is greater than 1 cm).
- Nails
- Scalp.
- Rarely in the face.
Usually the rash is of a symmetrical pattern, i.e. it affects both sides of the body equally.
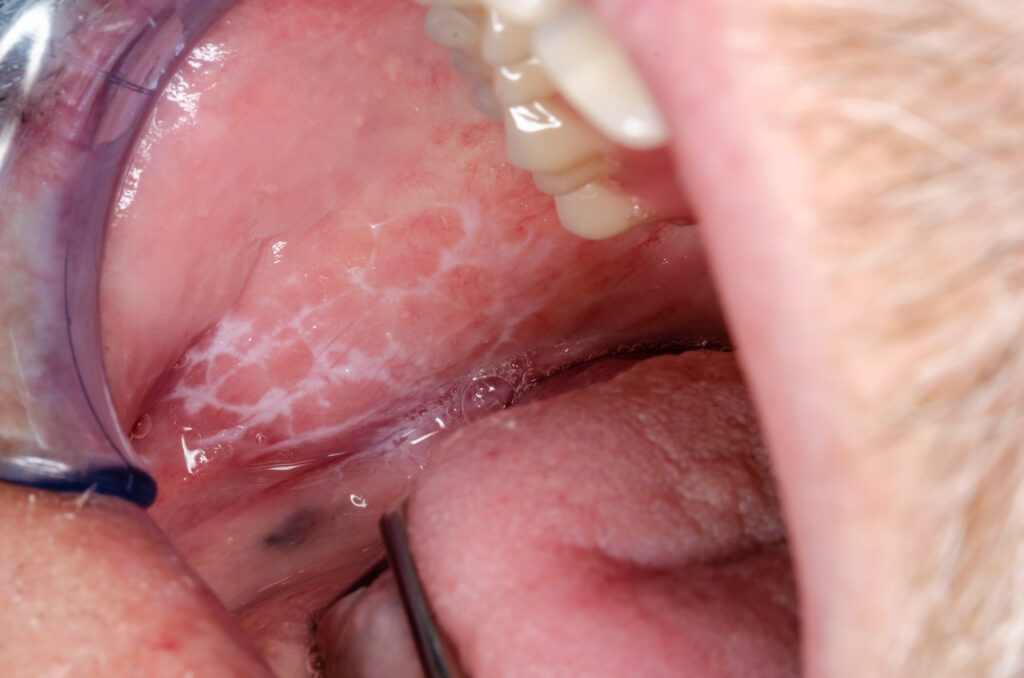
On the mucous membranes, however, lichen planus appears in the form of mesh-like or whitish lesions or pustules, which can cause discomfort. It can be located at the:
- Mouth
- Genital organs
Lichen planus is not contagious and occurs when the immune system unleashes an attack against its own cells: the cause of this abnormal immune reaction is not known with certainty, but there appears to be no familiarity.
Lichen planus can be triggered by various chemical, biological or pharmacological agents (especially β-blockers, NSAIDs, ACE inhibitors, sulphanilureas, antimalarials, penicillamine and thiazides). Recently, associations with liver failure related to hepatitis C, primary biliary cirrhosis and other forms of hepatitis have been reported.
USEFUL ADVICE
Lichen planus is a chronic and recurrent disease. Acute episodes tend to resolve in 6-12 months, but can last up to 2 years. It is advisable to see a doctor to start treatment to eliminate the itching and facilitate healing of the skin.
Corticosteroids are the most advised drugs for treating the inflammation related to lichen planus and consequently also the symptoms, especially itching.
There are no real guidelines to follow in order to keep this condition under control; however, the following can be useful:
- Reduce periods of high stress
- Self-diagnosis, paying particular attention to each new lesion and monitoring its evolution.
- Avoid stimulation and friction in the area in case of itching.
In the case of oral lichen, the following is recommended:
- stop smoking,
- reduce or eliminate alcohol consumption,
- avoid consumption of acidic and spicy foods, which can irritate the oral mucous membrane,
- take special care with oral hygiene by using toothpastes without strong aromas and avoiding the use of mouthwashes with alcohol.
